What is panel management?
Panel management is a process of proactively managing a defined population of patients, using EMR (electronic medical record) data to identify and respond to patients’ chronic and preventative care needs. The concept is simple: better information about patients leads to better care for patients.
The phases of panel management are a framework designed to support physicians in providing longitudinal, proactive care to patients. An accurate panel means physicians can easily track billings, improve workflows, improve communications with patients, and maintain a better work-life balance.
Panel management helps physicians:
-
Improve patient care and workflow efficiency through improve EMR processes.
-
Identify resource needs to help family doctors care for their patients.
-
Inform and plan proactive and preventative care.
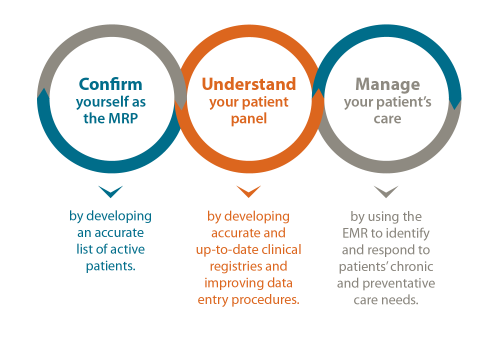
Panel management has three phases:
-
Empanelment assigns patients to individual primary care providers. Having an accurate list of active patients for each provider improves continuity of care and enables population-based care.
-
Panel clean-up involves creating registries that accurately reflect all patients within the panel who have a specific diagnosis and are properly coded with the correct ICD-9 code.
-
Panel optimization involves using updated data to implement proactive care goals using decision support tools in the EMR.
Practice support coaches can create and support manageable steps to help physicians optimize their EMR data as they work through the phases of panel management.
How do I get started?
Contact your practice support coach, or email us at [email protected], or submit a service request here and get started.
How long does panel management take?
Each phase could take up to 15 hours of physician or staff time to complete. The total time commitment may be up to 12 months.
For resources to develop and submit your list of Empanelled Patients to the Provincial Attachment System (PAS) Panel Registry, click here. These resources are intended to support longitudinal physicians on the LFP Payment Model, fee-for-service, and Alternative Payment models..
Panel management education opportunities
- Panel Management Small Group Learning Sessions
-
These sessions provide a group setting where PSP Coaches lead family physicians through the phases of panel management. EMR-specific sessions will be offered for Oscar, TELUS MedAccess, Intrahealth Profile, and MOIS.
Read more about Panel Management Small Group Learning Sessions.
- Panel Management Course with the University of the Fraser Valley
-
The Panel Management Program is a collaboration between the FPSC and the University of the Fraser Valley. The program is designed for medical office staff seeking to develop panel management skills to enhance their clinic's processes and workflows.
